Pancreatitis Causes and Treatment Options You Need to Understand
Pancreatitis is inflammation of the pancreas — a gland responsible for producing digestive enzymes and hormones including insulin. When the pancreas becomes inflamed, its own digestive enzymes begin breaking down pancreatic tissue, causing significant pain and potentially serious complications. Pancreatitis can be acute, occurring suddenly and resolving with treatment, or chronic, developing progressively over years. Understanding what causes pancreatitis, how it is diagnosed, and what pancreatitis treatment involves is essential for anyone at risk or experiencing symptoms.
What Is Pancreatitis?
Pancreatitis occurs when digestive enzymes produced by the pancreas become prematurely activated and begin attacking the pancreatic tissue itself rather than waiting to enter the small intestine. This self-digestion triggers inflammation, swelling, and in severe cases, tissue death and hemorrhage. The pancreas serves two critical functions — producing digestive enzymes and manufacturing hormones including insulin and glucagon — both of which are disrupted during active pancreatitis.
Acute vs. Chronic Pancreatitis
Acute pancreatitis develops suddenly and most cases resolve within days to weeks with appropriate medical support. The majority of acute pancreatitis cases are mild, but approximately 20 percent are severe, with potentially life-threatening complications. Chronic pancreatitis is a progressive, irreversible condition in which repeated or sustained inflammation causes permanent scarring of the pancreas. Over time, chronic pancreatitis impairs both the digestive and hormonal functions of the gland, leading to malnutrition and diabetes.
Common Causes of Pancreatitis
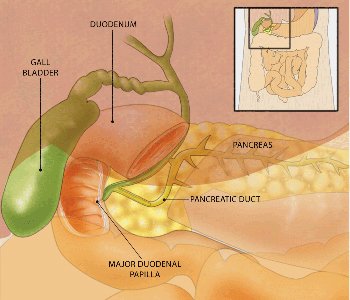
The two most common causes of pancreatitis are gallstones and alcohol use, accounting for approximately 80 percent of acute cases combined. Gallstone pancreatitis occurs when a stone obstructs the shared opening of the bile duct and pancreatic duct. Alcohol causes pancreatitis through direct toxic effects on pancreatic cells and by stimulating enzyme secretion. Other causes include hypertriglyceridemia, certain medications, abdominal trauma, hereditary conditions, autoimmune disease, and in many cases no identifiable cause — called idiopathic pancreatitis.
Symptoms of Pancreatitis
The hallmark symptom of pancreatitis is severe, persistent abdominal pain centered in the upper abdomen and often radiating through to the back. This pain typically worsens after eating and may be partially relieved by leaning forward. Nausea and vomiting are common, and the abdomen may be tender to palpation. Fever, rapid heart rate, and elevated white blood cell count indicate inflammation. In severe pancreatitis, patients may develop jaundice if there is associated bile duct obstruction.
Diagnosing Pancreatitis
Diagnosis of pancreatitis relies primarily on elevated serum amylase and lipase levels — pancreatic enzymes that spill into the bloodstream during pancreatic inflammation. Lipase is the more sensitive and specific marker. Imaging with CT scan confirms the diagnosis, assesses severity, and identifies complications such as pancreatic necrosis, pseudocyst formation, or abscess. MRI and endoscopic ultrasound provide additional detail about pancreatic and bile duct anatomy when needed.
Treatment of Acute Pancreatitis
Most cases of acute pancreatitis are managed with supportive care including bowel rest, aggressive intravenous fluid resuscitation, pain control, and monitoring for complications. Early oral feeding when tolerated improves outcomes compared to prolonged fasting. Antibiotics are reserved for confirmed infectious complications rather than routine use. The gallbladder should be removed before hospital discharge in patients whose pancreatitis was caused by gallstones to prevent recurrence of this potentially serious condition.
Severe Acute Pancreatitis and Complications
Severe acute pancreatitis involves organ failure, infected pancreatic necrosis, or other systemic complications and carries a significant mortality risk. Patients require intensive care monitoring, nutritional support through enteral feeding, and in the case of infected necrosis, minimally invasive or surgical drainage. ERCP may be urgently needed to remove an obstructing gallstone. Severe pancreatitis is a medical emergency that requires specialized multidisciplinary care.
Pancreatic Pseudocysts
A pancreatic pseudocyst is a fluid collection that forms adjacent to the pancreas after an episode of acute pancreatitis, typically developing two to four weeks after the initial event. Most pseudocysts resolve spontaneously, but those that are large, symptomatic, or infected require drainage. Endoscopic ultrasound-guided drainage — performed by a gastroenterologist — provides a minimally invasive alternative to surgical drainage for most pseudocysts, significantly reducing recovery time and complications.
Chronic Pancreatitis: Progressive Damage
Chronic pancreatitis develops when repeated inflammation causes irreversible fibrosis and destruction of pancreatic tissue. Alcohol use is the most common cause, followed by hereditary conditions and idiopathic factors. Patients with chronic pancreatitis experience recurrent or persistent abdominal pain, malabsorption from insufficient digestive enzyme production causing weight loss and fatty stools, and eventually diabetes from destruction of insulin-producing cells. Pancreatitis treatment in the chronic setting focuses on pain management and replacement of lost pancreatic function.
Pancreatitis Treatment in Chronic Cases
Pancreatitis treatment for chronic disease is multifaceted. Complete alcohol cessation is essential and the most impactful intervention in alcohol-related chronic pancreatitis. Pancreatic enzyme replacement therapy manages malabsorption and improves nutritional status. Pain management often requires a stepwise approach from non-opioid medications to opioids and potentially interventional procedures. Endoscopic procedures to decompress the pancreatic duct or address strictures can provide meaningful pain relief in selected patients.
Endoscopic Management of Pancreatitis
Gastroenterologists play a central role in managing pancreatitis complications through advanced endoscopic procedures. ERCP treats bile duct stones that precipitate gallstone pancreatitis and addresses pancreatic duct strictures in chronic disease. Endoscopic ultrasound guides drainage of pseudocysts and evaluates masses to differentiate pancreatitis complications from pancreatic cancer. These procedures provide effective, minimally invasive treatment for many pancreatitis complications that previously required surgery.
Diet and Pancreatitis Recovery
Diet plays an important role in both acute pancreatitis recovery and chronic pancreatitis management. During acute pancreatitis recovery, starting with small, low-fat meals and advancing gradually as tolerated is recommended. For chronic pancreatitis, a low-fat diet in multiple small meals daily reduces pancreatic stimulation and symptom burden. Alcohol must be eliminated completely. Patients with chronic pancreatitis often benefit from working with a dietitian to optimize nutrition while managing fat malabsorption.
Autoimmune Pancreatitis
Autoimmune pancreatitis is a rare, steroid-responsive form of chronic pancreatitis caused by IgG4-related disease or another immune-mediated mechanism. It can mimic pancreatic cancer on imaging, making accurate diagnosis critical. Characteristic features include diffuse pancreatic enlargement, elevated serum IgG4 levels, and associated involvement of other organs. Autoimmune pancreatitis responds dramatically to corticosteroid therapy, distinguishing it from other forms of chronic pancreatitis and from malignancy.
Pancreatitis and Pancreatic Cancer Risk
Chronic pancreatitis significantly increases the long-term risk of pancreatic cancer, particularly in patients with hereditary pancreatitis or prolonged chronic disease. The annual risk of pancreatic cancer in patients with longstanding chronic pancreatitis is low in absolute terms but meaningfully elevated compared to the general population. Patients with chronic pancreatitis require monitoring for concerning changes and should discuss surveillance strategies with their gastroenterologist.
Preventing Recurrent Pancreatitis
Preventing recurrent acute pancreatitis requires addressing the underlying cause. In gallstone pancreatitis, cholecystectomy prevents recurrence and should be performed promptly after recovery. In alcohol-related pancreatitis, sustained sobriety is essential. Treating hypertriglyceridemia with dietary modification and medication prevents triglyceride-induced pancreatitis. For patients with other identified causes, targeted management of the specific precipitant reduces recurrence risk significantly.
Getting Proper Care for Pancreatitis
Both acute and chronic pancreatitis require expert gastroenterology management. A gastroenterologist evaluates the cause and severity of pancreatitis, coordinates appropriate imaging and endoscopic procedures, manages complications, and guides long-term care for chronic disease. Patients who have experienced even a single episode of acute pancreatitis should receive follow-up care to prevent recurrence, address the underlying cause, and screen for complications including pseudocyst or pancreatic duct changes.
Call To Action
If you are experiencing digestive symptoms or are due for preventive screening, expert gastroenterology care can help. Learn more about available services or request an appointment with GI Associates today.
Citations
NIH – Pancreatitis
https://www.niddk.nih.gov/health-information/digestive-diseases/pancreatitis
Mayo Clinic – Pancreatitis
https://www.mayoclinic.org/diseases-conditions/pancreatitis
Cleveland Clinic – Pancreatitis Treatment
https://my.clevelandclinic.org/health/diseases/8103-pancreatitis
For education only, not medical advice.