What Causes GERD?
What Causes GERD?
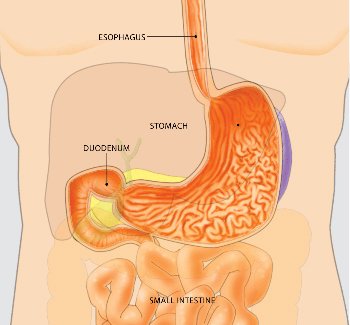
GERD is caused by a dysfunction of the lower esophageal sphincter (LES), a muscular ring that acts as a valve between the esophagus and stomach. When this valve weakens or relaxes abnormally, stomach acid can escape upward into the esophagus.
Common Triggers and Risk Factors
Several factors contribute to the development and persistence of GERD:
- Hiatal hernia: A condition in which part of the stomach pushes through the diaphragm, weakening the LES.
- Obesity: Excess abdominal fat increases pressure on the stomach, which can promote reflux.
- Smoking: Tobacco relaxes the lower esophageal sphincter (LES) and impairs saliva production, which normally helps neutralize stomach acid.
- Dietary choices: Spicy foods, caffeine, chocolate, alcohol, citrus fruits, and high-fat meals can all exacerbate acid reflux.
- Pregnancy: Hormonal changes and increased abdominal pressure can lead to temporary GERD.
- Medications: Some drugs, such as antihistamines, pain relievers, and blood pressure medications, may interfere with LES function.
- Delayed stomach emptying: When the stomach fails to empty properly, pressure builds, and reflux becomes more likely.
Understanding your triggers is key to managing GERD effectively.
Symptoms of GERD
GERD symptoms can range from mild to severe and may vary from person to person. Recognizing them early helps guide treatment and prevent complications.
- Heartburn: A burning sensation in the chest, especially after eating or when lying down.
- Regurgitation: Sour or bitter-tasting acid backing up into the throat or mouth.
- Chest pain: Often mistaken for heart issues, but typically related to acid irritation.
- Difficulty swallowing (dysphagia): May indicate inflammation or narrowing of the esophagus.
- Chronic cough or sore throat: Caused by acid irritating the throat or vocal cords.
- Hoarseness or laryngitis: Common in those with nighttime reflux.
- Feeling of a lump in the throat: A frequent sensation linked to esophageal inflammation.
If symptoms persist for several weeks, it’s essential to seek a medical evaluation to confirm GERD and rule out other potential conditions.
How to Find Relief from GERD
Relief from GERD typically involves a combination of lifestyle changes, medications, and in some cases, surgical intervention. Early intervention helps minimize long-term damage and discomfort.
Lifestyle Modifications
Adjusting daily habits can make a significant difference in symptom control:
- Eat smaller, more frequent meals to reduce stomach pressure.
- Avoid lying down for at least two to three hours after eating.
- Elevate the head of your bed by 6 to 8 inches to prevent nighttime reflux.
- Limit foods that trigger reflux, such as acidic, spicy, or greasy meals.
- Maintain a healthy weight, as excess pounds increase abdominal pressure.
- Quit smoking to support LES function and reduce irritation.
- Wear loose-fitting clothing around the abdomen to reduce pressure on the stomach.
Consistency with these habits is key for ongoing symptom relief.
Over-the-Counter Medications
Mild to moderate GERD symptoms often respond well to OTC treatments:
- Antacids: Provide quick, short-term relief by neutralizing stomach acid (e.g., Tums, Rolaids).
- H2 blockers: Reduce acid production for longer-lasting relief (e.g., famotidine, ranitidine*).
- Proton pump inhibitors (PPIs): More potent acid reducers that help heal the esophagus (e.g., omeprazole, lansoprazole).
*Note: Ranitidine was recalled in many markets due to safety concerns. Speak with your doctor about safe alternatives.
Prescription Treatments
For persistent or severe GERD, a healthcare provider may prescribe:
- Higher-dose PPIs or H2 blockers
- Prokinetic agents that help the stomach empty more effectively
- Medications to protect the esophagus or reduce inflammation
Treatment should always be tailored to the individual’s needs and monitored by a physician.
Surgical Options
Surgery is considered when lifestyle and medication aren’t enough, or when complications arise:
- Nissen fundoplication: A common procedure in which the top of the stomach is wrapped around the LES to strengthen it.
- LINX device: A ring of magnetic beads is placed around the lower esophageal sphincter (LES) to keep it closed while allowing food passage.
These procedures are usually reserved for patients with severe GERD or those who prefer to avoid lifelong medication.
Potential Complications of Untreated GERD
Leaving GERD unmanaged can result in serious health problems over time:
- Esophagitis: Inflammation of the esophagus, which can cause pain and bleeding.
- Esophageal strictures: Narrowing of the esophagus due to scar tissue, making swallowing difficult.
- Barrett’s esophagus: A precancerous condition in which the esophageal lining changes due to chronic acid exposure.
- Esophageal cancer: Rare, but individuals with long-standing GERD and Barrett’s are at higher risk.
Proper management not only improves quality of life but also prevents these complications.
Conclusion: GERD Is Manageable with the Right Approach
GERD can be a frustrating and disruptive condition, but with the right knowledge and a commitment to managing its causes, relief is achievable. By identifying personal triggers, making targeted lifestyle changes, and using appropriate medications or therapies, most individuals can effectively manage their symptoms and prevent complications.
If you experience frequent heartburn, regurgitation, or difficulty swallowing, it’s time to speak with a healthcare provider. With proper treatment and proactive care, GERD doesn’t have to control your life.